Napping Smarter – The Role of Nasal Airflow in Daytime Sleep Quality
Over short naps, your nasal airflow largely determines whether you wake refreshed or groggy. Optimize your nap by promoting nasal breathing and adding nasal strips to increase airflow, which can boost oxygenation and alertness and lower the risk of sleep fragmentation and daytime fatigue. Combine this with a myofunctional oral appliance like Pacivox: Myofunctional Oral Appliance & Nasal Breathing … to support your nasal patency and improve productivity and long-term wellness.
Key Takeaways:
- Clear nasal airflow enhances nap quality by reducing sleep latency and deepening restorative sleep stages; nasal dilator strips help keep passages open for better oxygenation during short daytime naps.
- Unobstructed nasal breathing shortens time to fall asleep and reduces fragmented sleep, making 20-30 minute power naps more effective for memory consolidation and alertness recovery.
- Including nose strips in a consistent pre-nap routine supports faster recovery, reduced grogginess, and improved daytime productivity and overall wellness.
Nasal anatomy and physiology
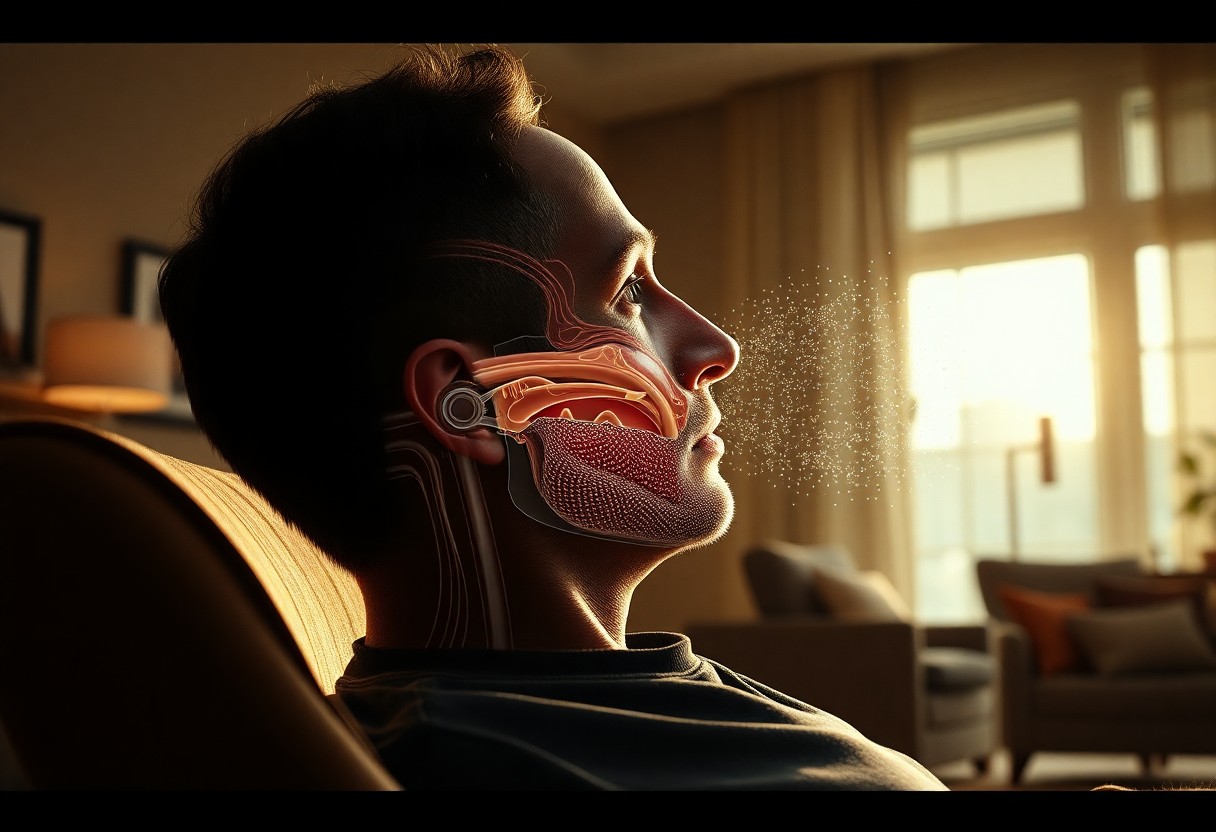
Your nose combines delicate mucosa, cilia and vascular turbinates to filter, warm and humidify air while shaping resistance that directly affects nap depth and continuity. Nasal nitric oxide supports airway defense and gas exchange, so when congestion or collapse raises resistance you may wake more easily. Integrating a nasal strip into your nap routine can measurably reduce resistance and help preserve the restorative benefits of short daytime sleep.
Structural determinants of airflow (nasal valve, turbinates, septum)
The narrowest region, the nasal valve, can account for up to 50% of total nasal resistance, while turbinates regulate surface area and humidification; a deviated septum further redirects flow. When turbinates are hypertrophied or the valve collapses on inspiration, you get turbulence, higher work of breathing, and more mouth breathing. Using nasal strips lifts the lateral nasal wall to widen the valve and reduce resistance, helping you keep nasal breathing during naps.
Respiratory control during sleep and the nasal vs. oral pathway
During sleep your brain reduces pharyngeal muscle tone and breathing shifts toward the path of least resistance; if the nose is obstructed you’ll default to oral breathing, which increases airway collapsibility and can provoke snoring or arousals. Nasal breathing preserves humidified, NO-rich airflow and tends to stabilize ventilation, so when you use a nasal strip you encourage the preferable nasal route and protect nap continuity and oxygenation.
Brainstem-driven patterns change across NREM and REM: NREM favors regular, lower-rate breathing while REM increases variability and upper-airway susceptibility. In the supine position nasal resistance often rises, increasing the chance you’ll switch to mouth breathing and fragment a short nap. Practical example: applying a nasal strip before a 20-30-minute nap reduces lateral wall collapse and helps maintain nasal breathing, supporting deeper, more productive daytime sleep.

How nasal airflow influences daytime nap quality
Nasal patency directly shapes how efficiently you descend into restorative nap states: when your nose is clear you more easily reach light and slow-wave stages within a 10-30 minute window, whereas obstruction fragments sleep and shortens deep-sleep minutes. Using a nasal strip as part of an optimized nap routine can increase nasal airflow and reduce breathing effort, helping you get measurable benefits from brief naps and avoid wasted time from repeated wake-ups.
Effects on sleep continuity, microarousals, and sleep-stage architecture
Upper-airway resistance increases the frequency of microarousals, interrupting transitions into N2/N3 and reducing consolidated slow-wave minutes; studies report that improving nasal airflow reduces respiratory-related arousals and improves continuity. For naps specifically, increased continuity means you’re more likely to accumulate the 10-30 minutes of stable N2/N3 needed for alertness gains; adding a nasal strip before a scheduled nap often lowers nasal resistance by ~15-20% in clinical reports, which helps preserve sleep-stage architecture.
Consequences for post-nap cognition, alertness, and mood
If your nasal breathing is impaired you’ll frequently see blunted post-nap gains: reduced alertness, slower reaction time, and worsened mood compared with clear-nosed naps. Short naps (10-20 minutes) reliably boost vigilance and motor speed, while longer naps (60-90 minutes) aid declarative memory and creativity; using a nasal strip increases the odds that your chosen nap length delivers those specific cognitive outcomes rather than leaving you groggy.
Practical evidence shows that optimizing airflow before a nap changes outcomes: you’ll notice faster sleep onset, fewer awakenings, and stronger immediate performance effects on tasks requiring attention. For example, when you pair a 20-minute power nap with a nasal strip in a noisy office or travel setting, you reduce breathing effort and increase the likelihood of gaining the typical 20-40 minute alertness window post-nap; this makes nasal strips an effective, low-cost tool in a productivity-focused nap routine.
Common nasal impediments that degrade naps
Several nasal issues-congestion, allergic rhinitis (affecting ~10-30% of adults), and structural problems-regularly fragment daytime naps by raising airway resistance and provoking micro-arousals. You can often reduce their impact with targeted tactics; adding a nasal dilator strip to your optimized nap routine commonly boosts nasal airflow and nap productivity. Severe obstruction may still require ENT evaluation.
Congestion, allergic rhinitis, and anatomical obstruction
If you’re congested from a cold or seasonal allergies, nasal resistance climbs and naps become shallow and fragmented. Structural factors-deviated septum, turbinate hypertrophy, nasal polyps-produce persistent blockage; septal deviations are present in a majority of adults to some degree. Short-term fixes like saline, intranasal antihistamines, or a nasal strip can yield measurable airflow gains (studies report up to ~30% increases), but persistent obstruction needs specialist assessment.
Positional and environmental contributors (humidity, allergens)
Your position and room conditions can change nasal patency within minutes: lying flat promotes venous engorgement and congestion, while low humidity dries mucosa and high humidity encourages dust mites and mold. Adjusting posture before a 10-30 minute nap and controlling the room environment helps preserve airflow; pairing those steps with a nasal strip often sustains clearer breathing and better nap returns.
You can act on specific measures: keep humidity between 40-50% with a hygrometer and humidifier/dehumidifier, wash bedding weekly at ≥60°C to lower dust-mite load, and run a HEPA purifier. Elevating your head 10-15° or choosing back-position naps and using a saline spray 10 minutes prior clears mucus, and a nasal strip then helps maintain that improved airway for a restorative 20-30 minute nap.
Assessing nasal airflow and nap outcomes
When assessing how nasal airflow affects your naps, combine subjective reports with objective sensors to link breathing to outcomes. Use the Epworth Sleepiness Scale (0-24) and Karolinska (1-9) alongside nasal airflow monitors (L/min), acoustic rhinometry (cross-sectional area in cm²) and pulse oximetry (SpO2). If you’re testing nose strips as part of an optimized routine, track pre/post measures and watch for SpO2 falls ≥3-4% or ESS >10, which warrant medical attention.
Subjective tools (diaries, sleepiness scales)
You should keep brief nap diaries logging time-to-sleep, duration, perceived nasal blockage and post-nap alertness. Standard scales like the Epworth Sleepiness Scale (>10 suggests excessive daytime sleepiness) and Karolinska Sleepiness Scale (1-9) let you quantify change; rate sleepiness immediately before and after naps. Pair entries with nose-strip use to see if perceived airflow and daytime productivity improve over 1-2 weeks.
Objective measures (nasal airflow sensors, rhinometry, oximetry)
Objective tools give measurable endpoints: nasal airflow sensors report flow in L/min and waveform patterns, acoustic or active anterior rhinometry quantifies cross-sectional area in cm², and pulse oximetry tracks SpO2 and oxygen desaturation index (ODI). Use pre/post nap comparisons to evaluate interventions like nose strips; a consistent increase in nasal flow or cross-sectional area of >10-20% often translates to better nap efficiency. Flag SpO2 drops ≥3-4% or persistent low baseline SpO2 for clinical follow-up.
For practical testing, record a 5-minute seated baseline, then a standardized 20-30 minute nap with simultaneous nasal flow (sampling ≥50 Hz for waveform detail), rhinometry before/after, and continuous oximetry. Compare mean nasal flow (L/min), minimal cross-sectional area (cm²) and ODI; concordant improvements indicate a true physiological benefit from nose strips. Device literature and trials report nasal dilator strips increasing valve area by approximately 10-30%, and you’re most likely to see productivity gains when objective flow rises alongside lower KSS/ESS scores. Escalate care if you observe recurrent SpO2 <90% or sudden ODI spikes.
Interventions to optimize nasal airflow for better naps
Use a layered approach: combine simple behavioral tweaks, device options like external nasal strips, and targeted medical measures to maximize nap airflow and productivity. For evidence-based context, see Can napping make you smarter? | Cognitive Vitality. In practice, you can pair a nasal strip with a 10-20 minute nap, a brief saline rinse, and a humidifier set to 30-50% to improve subjective breathing and alertness.
Behavioral and environmental strategies (positioning, humidification, nasal-breathing training)
Start by elevating your head 15-30° to reduce nasal congestion and avoid face-down positions that compress the nasal passages. Run a humidifier at 30-50% relative humidity to prevent mucosal drying. Practice 5 minutes of slow nasal-only breathing before you nap to lower respiratory rate and prime airway patency; athletes report faster recovery when they use brief nasal-breathing drills pre-rest.
Medical and device options (saline, topical therapies, nasal strips, oral appliances)
Try isotonic saline (0.9%) rinses or sprays to clear mucus before a nap and consider intranasal steroids for chronic inflammation (effects in 1-3 weeks). Use topical decongestants only for up to 3 days to avoid rebound congestion (rhinitis medicamentosa). Include an external nasal strip as part of your nap routine to increase perceived airflow; oral appliances are reserved for diagnosed sleep apnea, not routine napping.
For practical use, apply the nasal strip across the bridge about 2 minutes before lying down and press for 10 seconds; combine with a quick saline spray and a humidifier set near 40% for best effect. Small studies and clinical reports show nasal strips improve subjective airflow and snoring metrics, and you should consult ENT if obstruction persists despite these measures or if you suspect sleep-disordered breathing.

Integrating airflow optimization into an effective nap routine
You should make nasal airflow a routine step: apply a low-cost nose strip before lying down, darken the room, set a 20-30 minute timer, and note changes in sleep latency and post-nap alertness. If you want deeper context about napping and respiratory outcomes consult Daytime napping and increased risk of incident respiratory …. Using a strip often reduces resistance enough to improve oxygenation and ease quick sleep onset.
Timing, duration, and nap type selection informed by nasal status
If your nose feels blocked favor a 10-20 minute power nap to avoid deep-sleep inertia; when a strip restores patency you can extend to 30 minutes for light slow-wave entry or schedule a 60-90 minute nap only early afternoon (13:00-15:00) for full-cycle recovery. You should track how each duration affects your wakefulness and productivity across several trials to find your sweet spot.
Combining interventions with nap hygiene to maximize productivity
Pair a nose strip with a cool 18-21°C room, an eye mask, white noise at ~40-50 dB, and a 20-minute alarm; you should use saline spray pre-nap if congested and avoid caffeine within 90 minutes. Together these measures shorten sleep latency and increase the odds you wake refreshed rather than groggy.
Use a simple pre-nap protocol: 5 minutes saline spray if needed, apply the strip and wait 2-3 minutes for adhesion, dim lights and lower temperature to ~19°C, set a 20-minute timer, and cue 40-50 dB brown/white noise. If you need deeper restoration repeat a 60-90 minute nap only once per day and test strip use across sessions. Be alert to persistent nocturnal snoring or daytime sleepiness-if symptoms persist you should consult a clinician to rule out obstructive sleep apnea before relying solely on strips.
Final Words
On the whole, you can improve daytime sleep quality and post-nap alertness by optimizing nasal airflow; simple measures like using nasal strips, controlling room environment, and timing short naps help you fall asleep faster, reduce snoring, and wake more refreshed. Incorporating nose strips into your nap routine is an easy, evidence-informed step that supports productivity and overall wellness when combined with consistent nap timing and light-management strategies.
FAQ
Q: How does nasal airflow affect the quality of a daytime nap?
A: Nasal airflow supports smoother, more stable breathing during sleep, which reduces micro-awakenings and improves oxygen exchange. When nasal resistance is low, you’re less likely to switch to mouth breathing, snore, or experience brief arousals that fragment sleep stages. For short naps (10-30 minutes) this means clearer post-nap alertness and better cognitive rebound; for longer naps that include slow-wave or REM sleep, improved airflow helps preserve deeper restorative stages rather than interrupting them with brief wake-ups.
Q: Can nasal strips make my naps more productive and beneficial for wellness?
A: Yes-external nasal strips can increase nasal valve opening and reduce resistance, making breathing easier while you nap. By promoting steadier nasal breathing they can lower the chance of snoring and small sleep disruptions, so you wake feeling more refreshed and mentally sharp. When combined with good nap timing and environment, nose strips are a simple, noninvasive tool to enhance the restorative and performance benefits of daytime sleep.
Q: How should I include a nose strip in an optimized nap routine, and are there any precautions?
A: Clean and dry the nose area, apply the strip according to the product directions (press to the bridge so it adheres securely), then lie down in a dark, cool, quiet place and set a timer for your target nap length (10-30 minutes for a power nap; ~90 minutes for a full sleep cycle). Combine the strip with other habits: dim lighting, minimal caffeine beforehand, a comfortable pillow and gentle white noise if needed. Remove the strip slowly after waking. Avoid using strips if you have facial skin irritation at the application site, known adhesive allergy, or severe nasal obstruction; consult a healthcare provider if you have chronic nasal congestion, frequent loud snoring, or suspected sleep apnea before relying on over-the-counter nasal aids.
